Rooted in Care: Landscape Architecture for Cognitive Health
Project overview
This project explores how landscape design can serve as a therapeutic tool to support individuals living with neurodegenerative conditions—such as Dementia, Alzheimer’s, and Parkinson’s disease—by helping delay cognitive decline, encouraging physical activity, and enhancing overall well-being.
Context
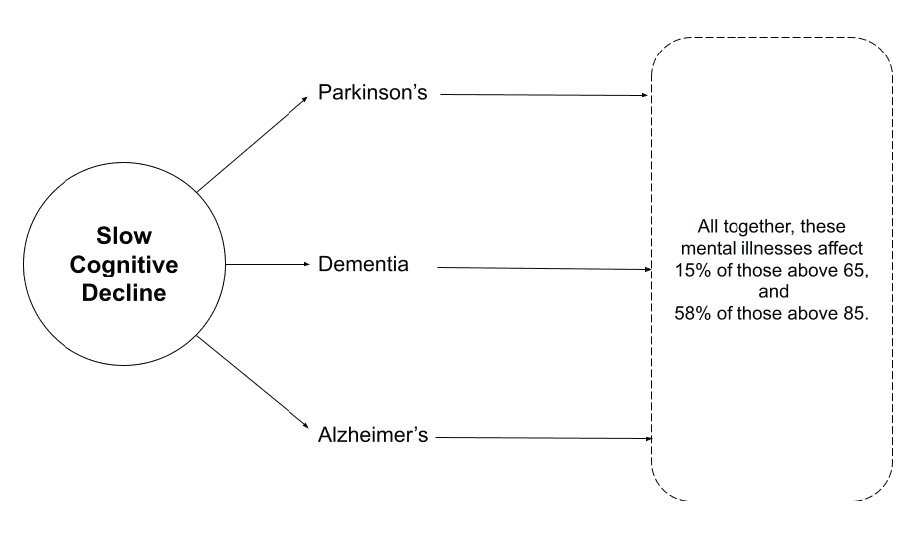
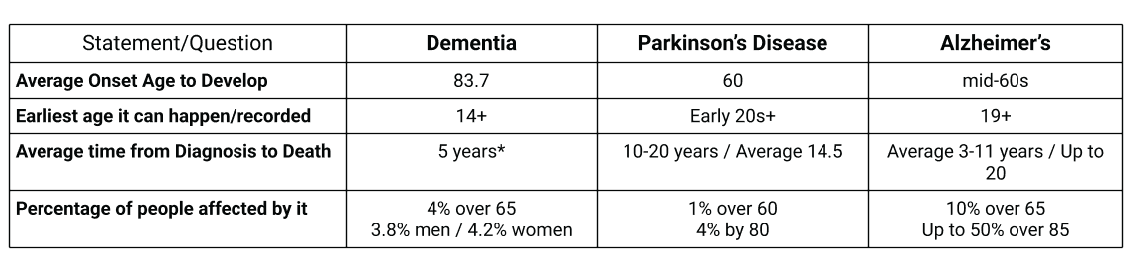
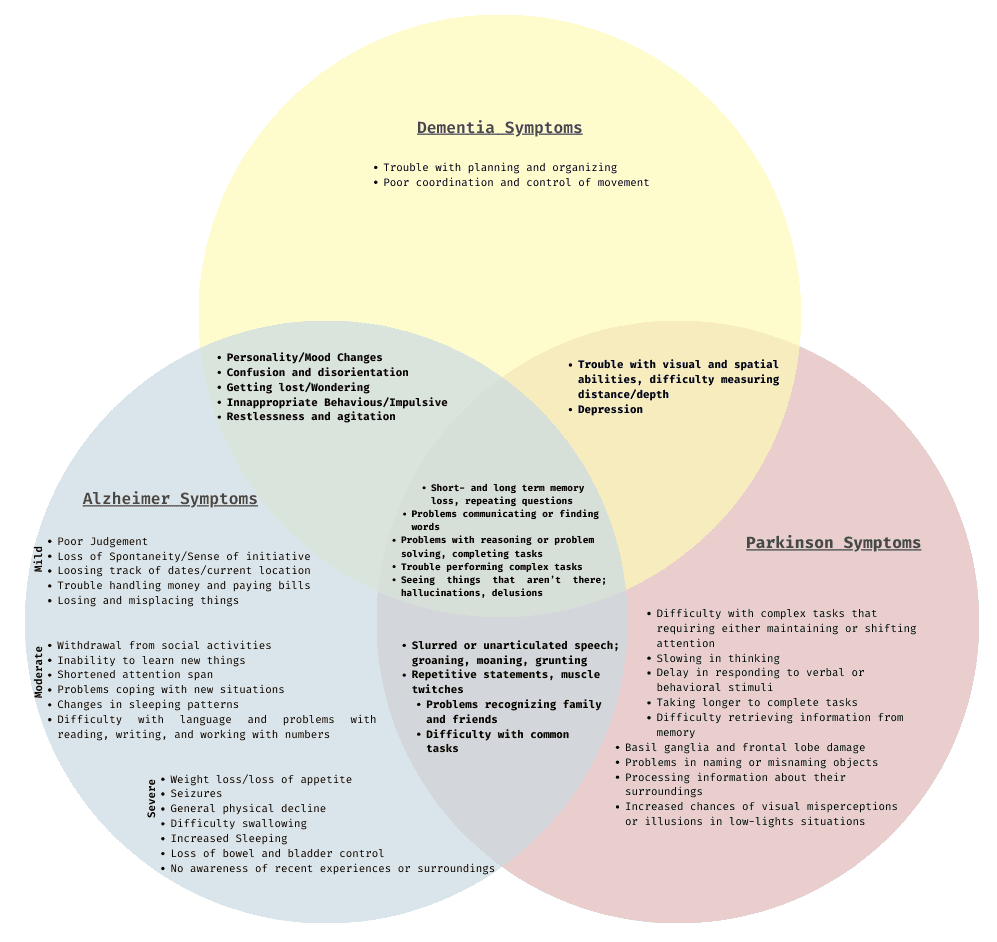
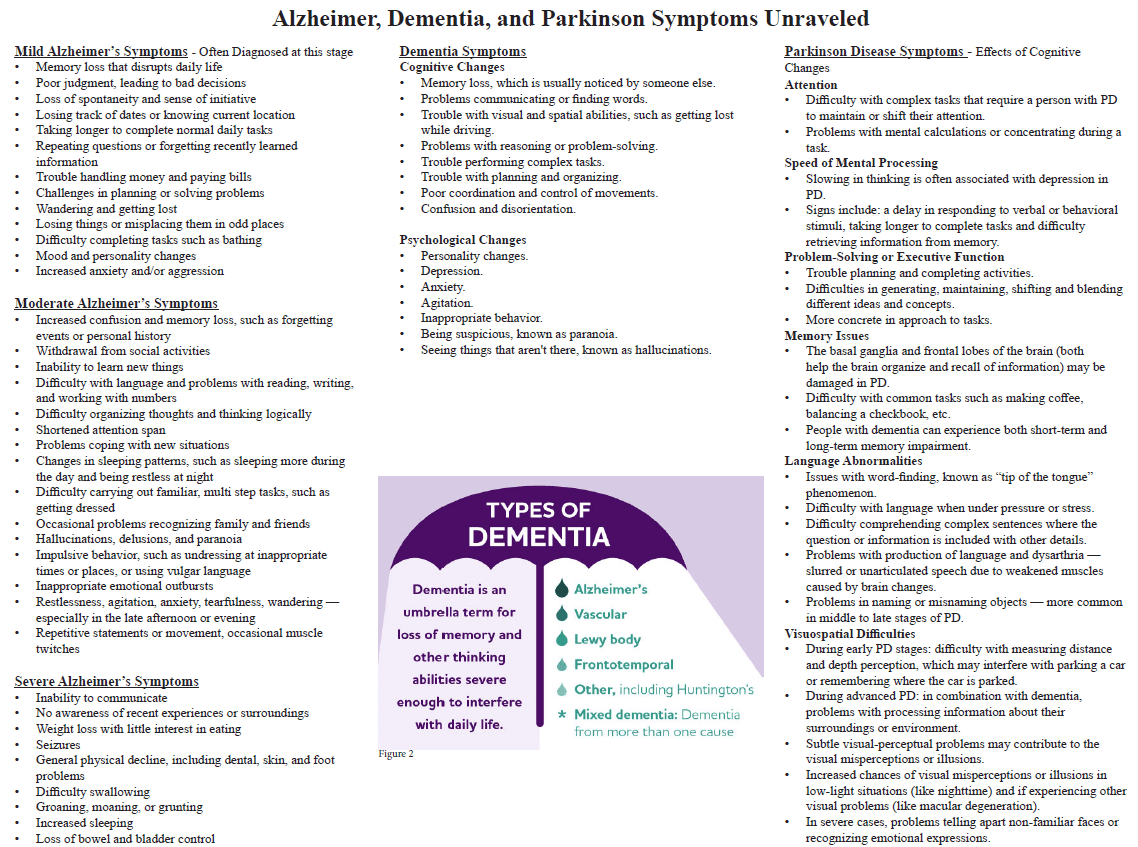
Dementia is the loss of cognitive functioning — thinking, remembering, and reasoning — and behavioral abilities to such an extent that it interferes with a person’s daily life and activities.
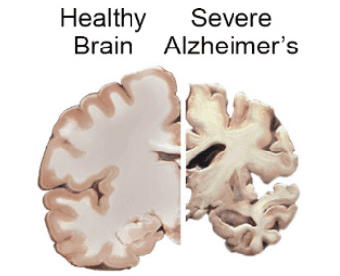
Alzheimer’s disease is a brain disorder that slowly destroys memory and thinking skills, and eventually, the ability to carry out the simplest tasks.
Alzheimer’s is currently ranked as the 7th leading cause of death in the United States and is the most common cause of dementia among older adults.
Parkinson disease causes physical symptoms at first. Problems with cognitive function, including forgetfulness and trouble with concentration, may start later. As the disease gets worse over time, about 4 in 5 people develop dementia.
Research Question
How can landscape elements enhance patients wellbeing and delay the decline of memory disorders and their respective cognitive impairments?
How can landscape design be naturally incorporated for the benefit of patients suffering with Dementia, Alzheimers and Parkinsons?
How can designing a facility based on outdoor recovery provide a more comfortable space for patients going through distress?
How can being exposed to natural environments encourage brain stimulation for patients in cognitive decline?
Goals and Objectives:
Create a landscape that positively impacts mental health.
Use research of programming and natural spaces to integrate impactful therapeutic landscapes for patients.
Include natural, researched solutions into the space designed.
Create a landscape that promotes a sense of place and recovery for patients in cognitive decline.
Research elements that provide a pragmatic effect to patients’ perception of the space and that provide an extra boost to help slow the cognitive decline.
Use research of programming and natural spaces to integrate impactful therapeutic landscapes to patients.
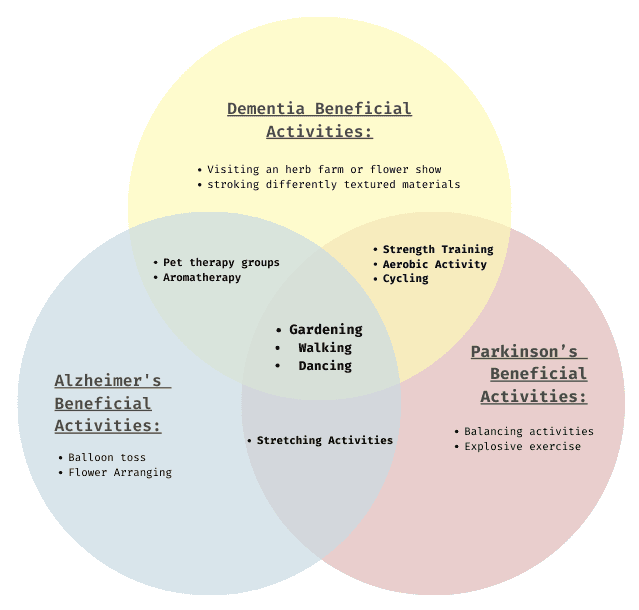
Utilize programming and landscape elements to promote beneficial physical activity for patients.
Use case study analysis and research about activities that positively impact patients cognitive decline with the mentioned mental illnesses to incorporate meaningful and impactful activities through strategic design into the programming.
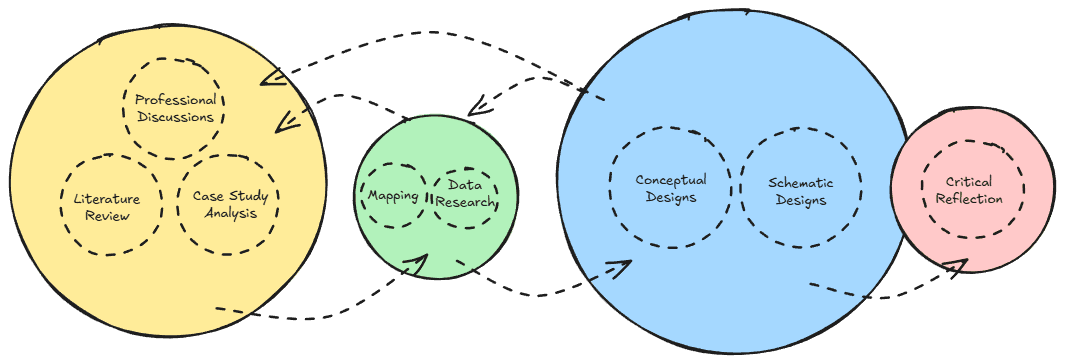
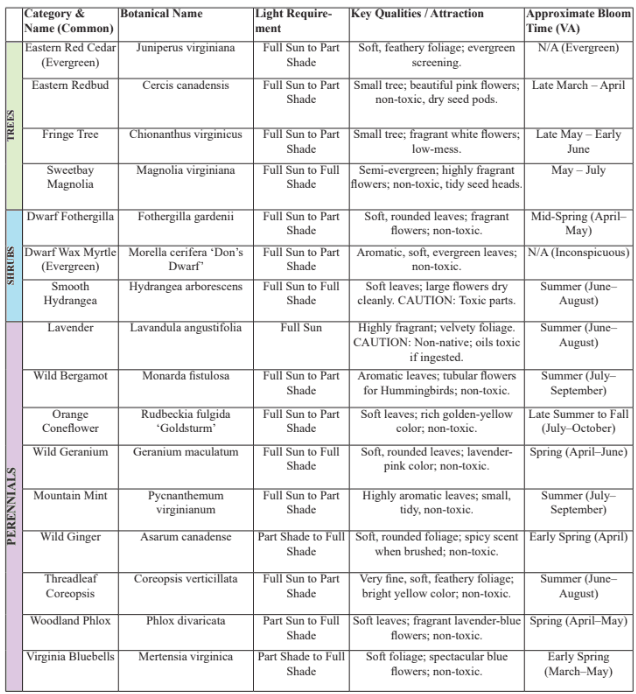
Toolkit:
Formulated from continuous research that can be found at the bottom of the page.
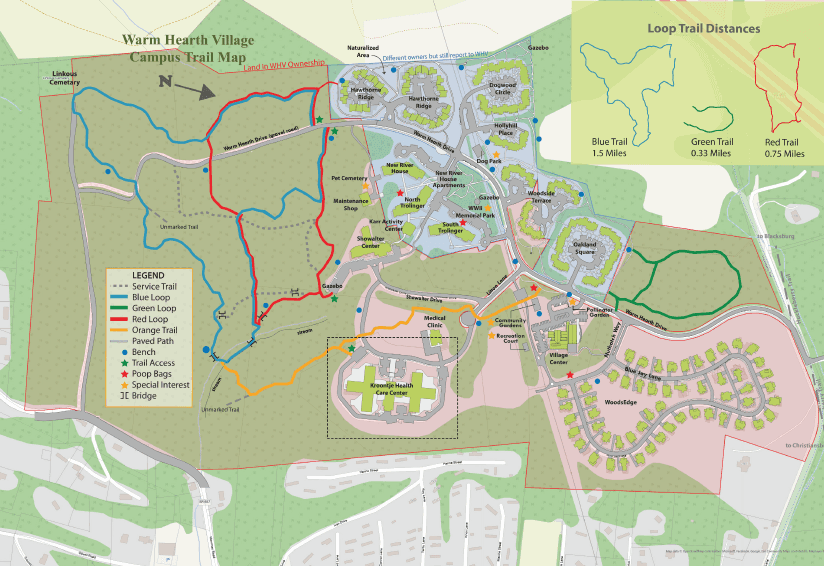
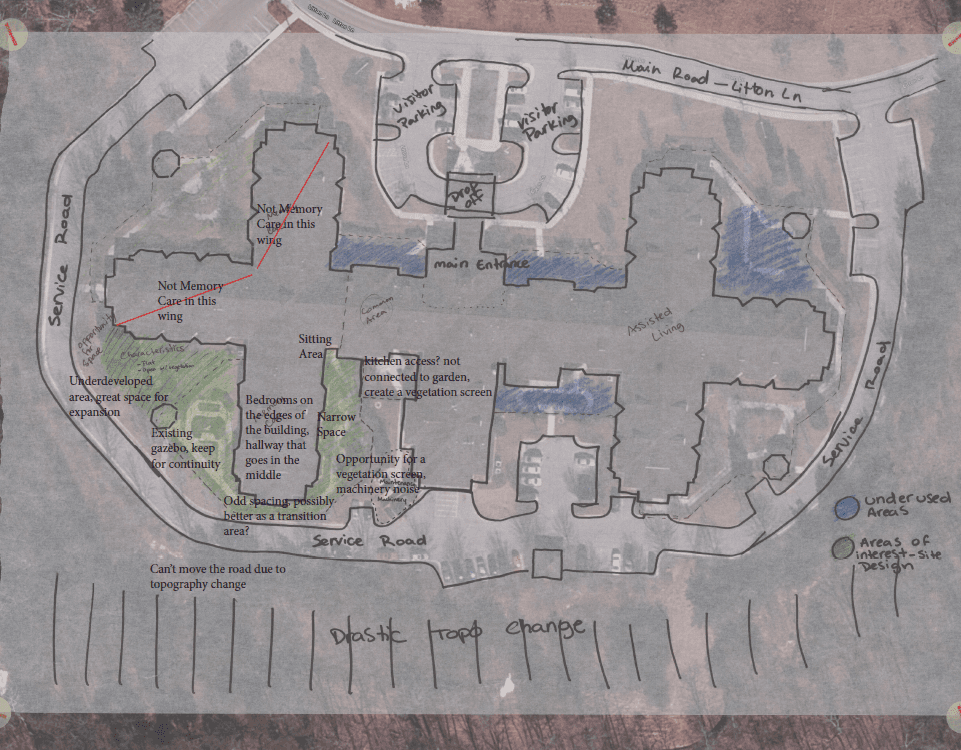
Site location within Warm Hearth Village
More information about the facility chosen and the site analysis done is towards the bottom of the page.
Design Concept
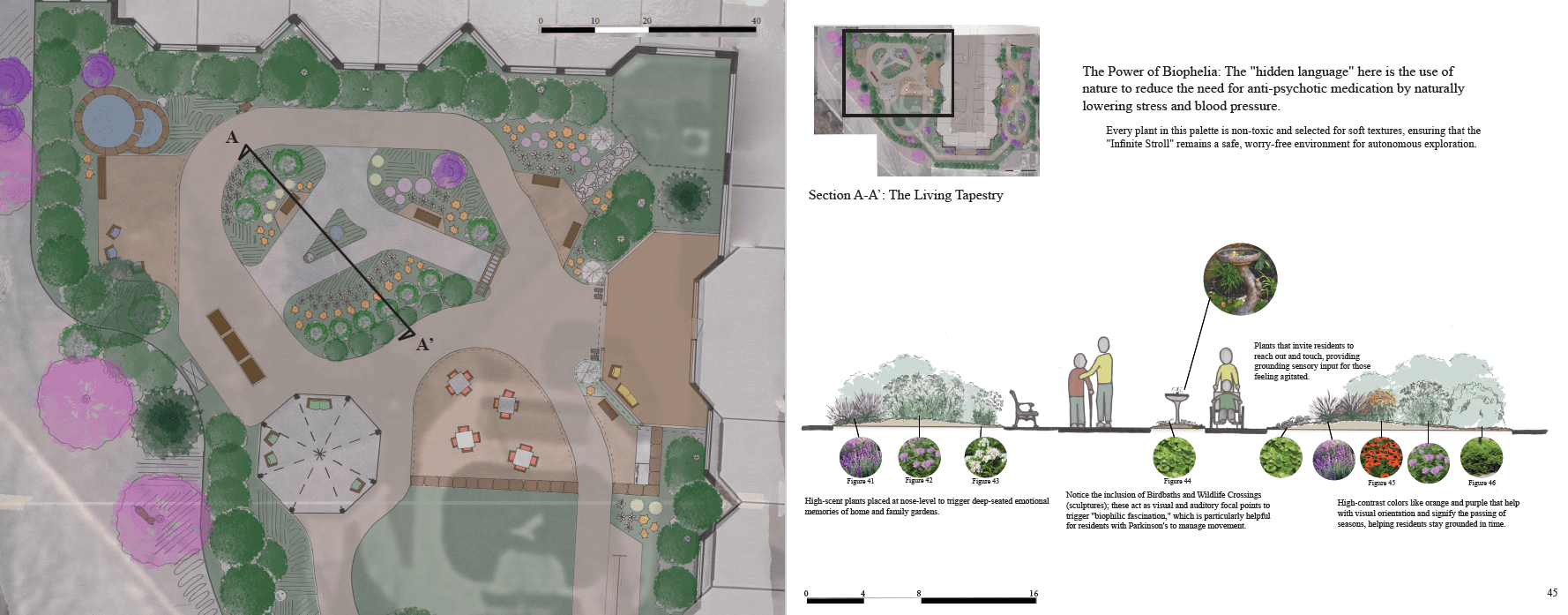
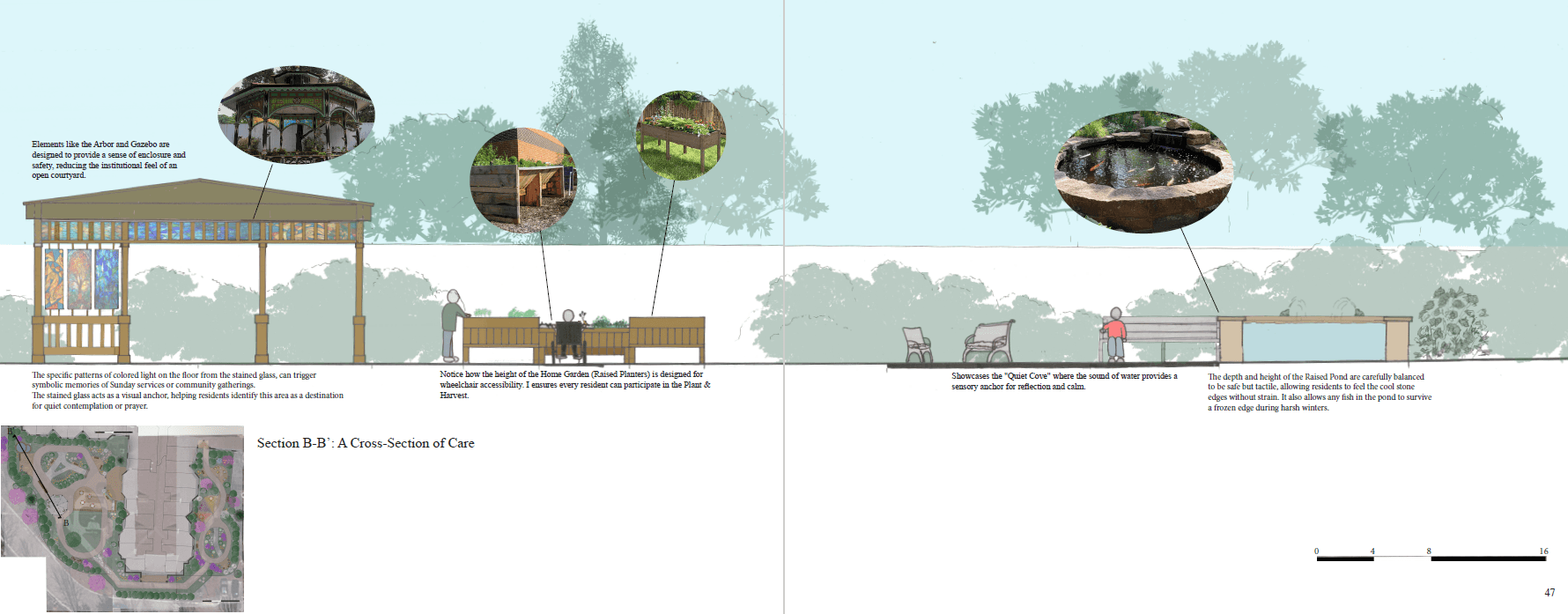
The garden is not just a space but a weaving of different sensory spaces (scents, sounds, and rituals) that residents can pick up to reconnect with their past.
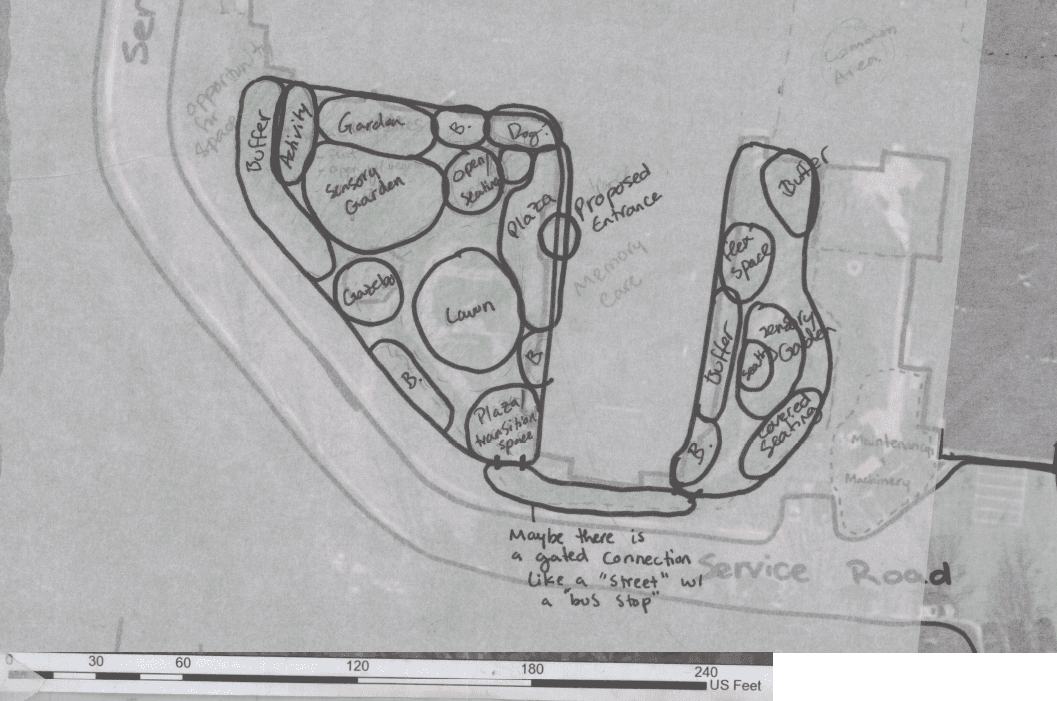
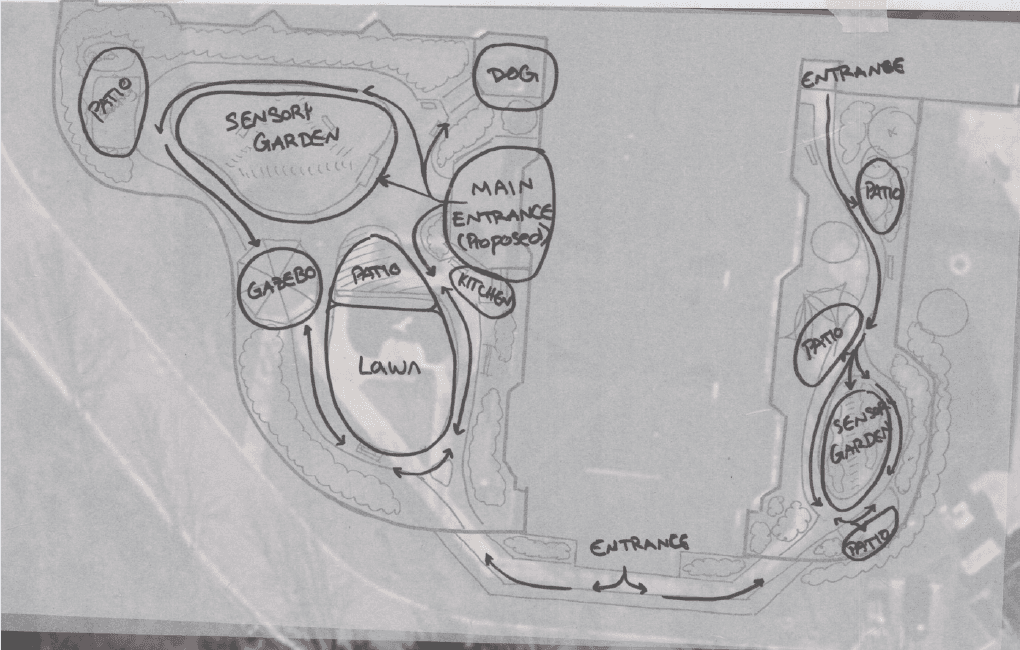
After multiple iterations trying to figure out which layout worked best, this is the last one that was closest to the final design. Since then it changed slightly once it was moved to site design.
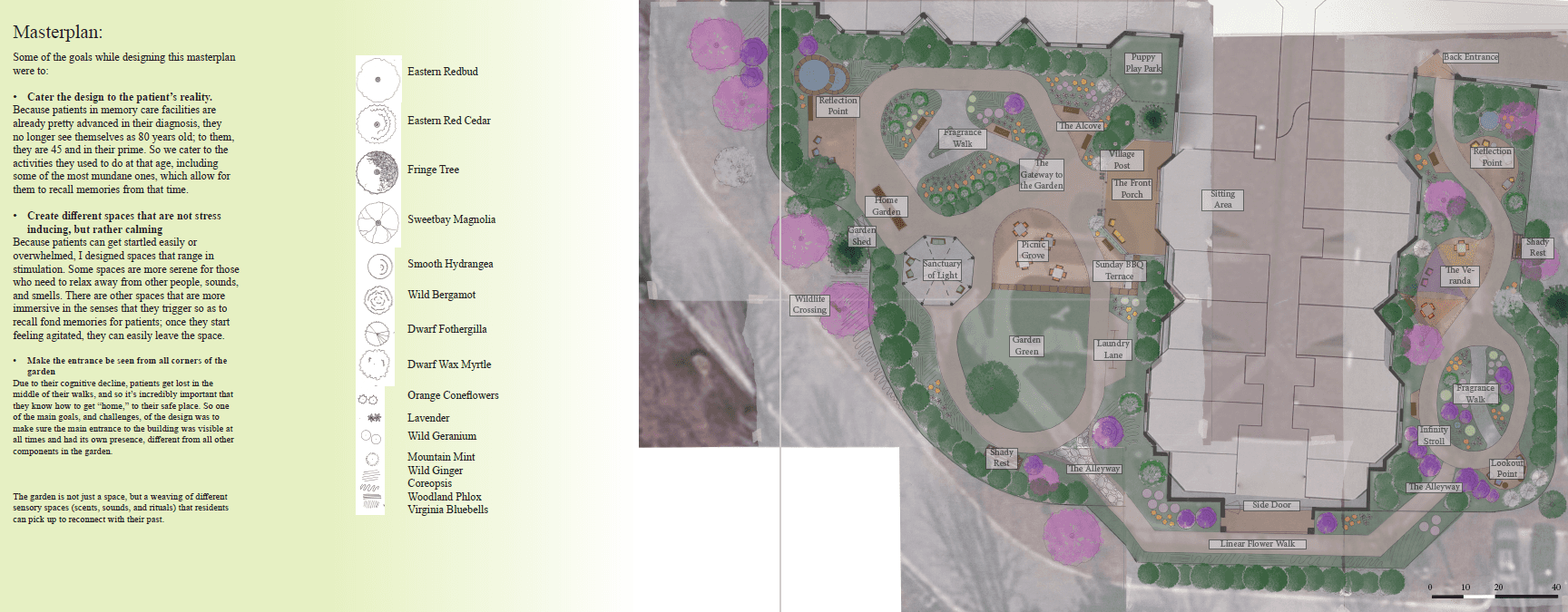
Final Design
Conceptual Layers and Diagrams:
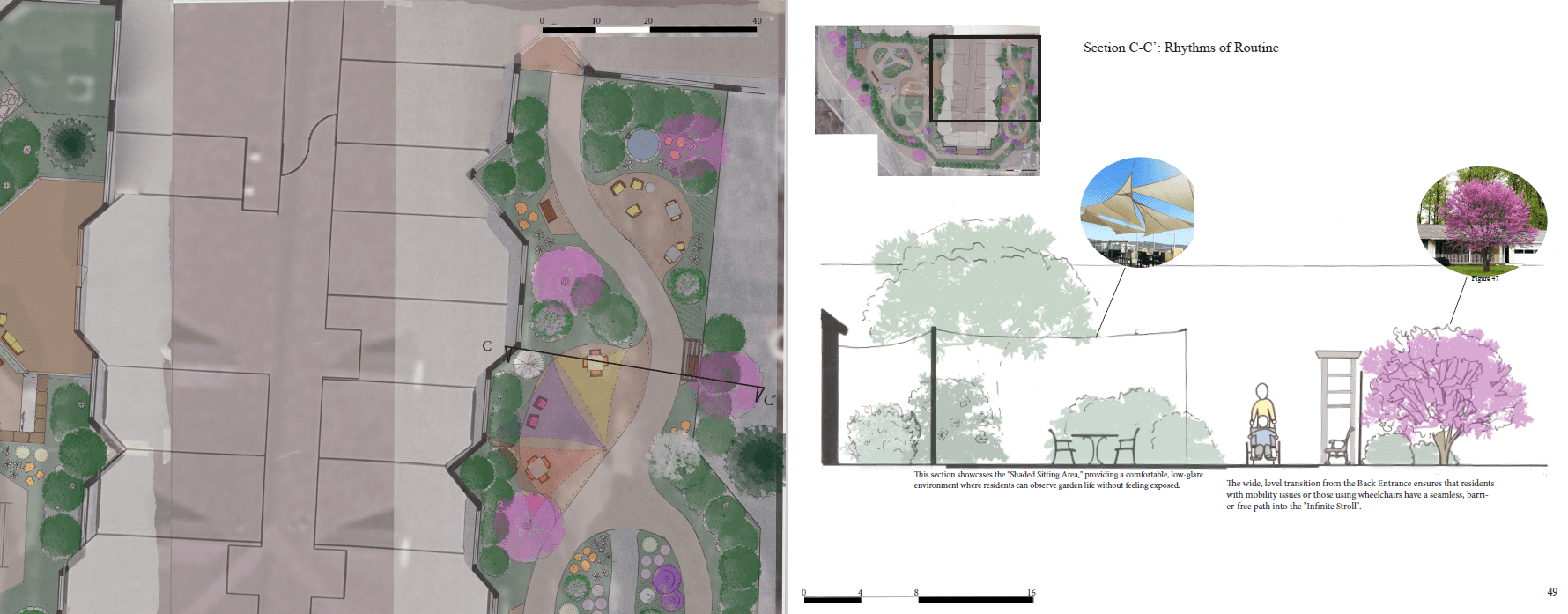
Spatial Diagram: A layout that uses looped pathways to encourage autonomous exploration while naturally guiding residents back to communal hubs.
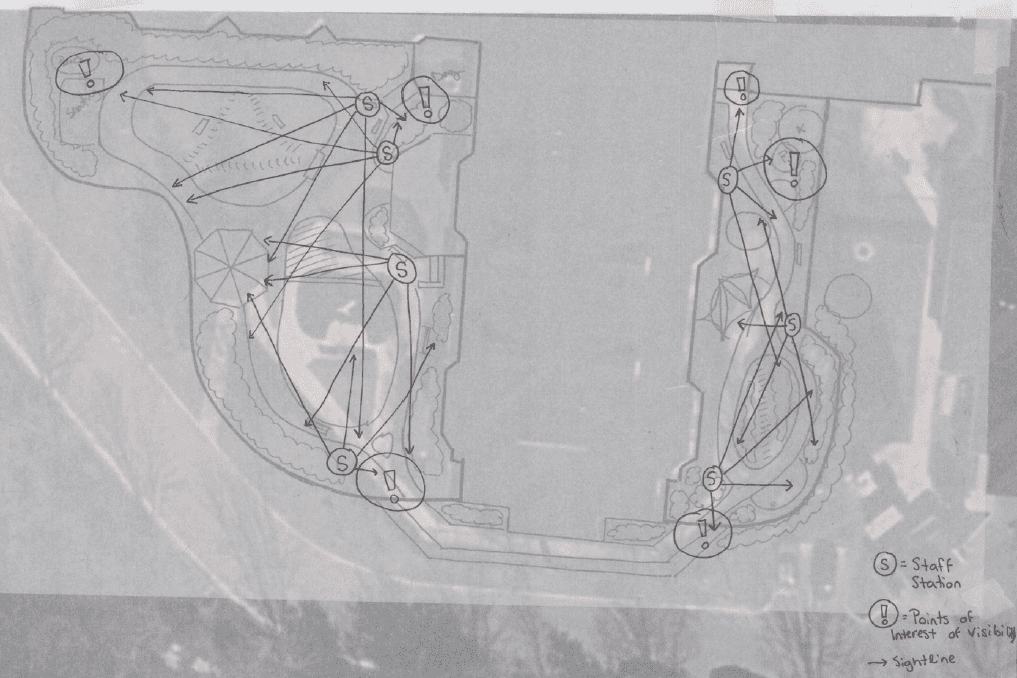
Safety Sightlines: Strategically mapped visual corridors that allow staff to provide unobtrusive supervision while maintaining the resident’s sense of privacy and independence.
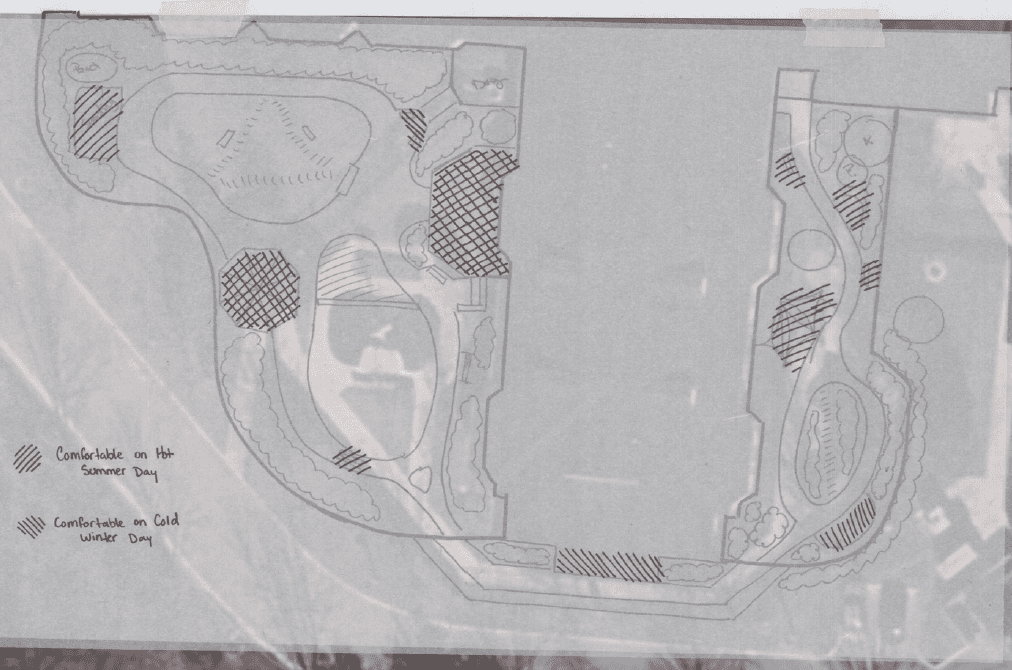
Micro Climates: A study of seasonal sanctuary points, mapping areas of natural warmth and cooling shade to support year-round engagement with the outdoors.
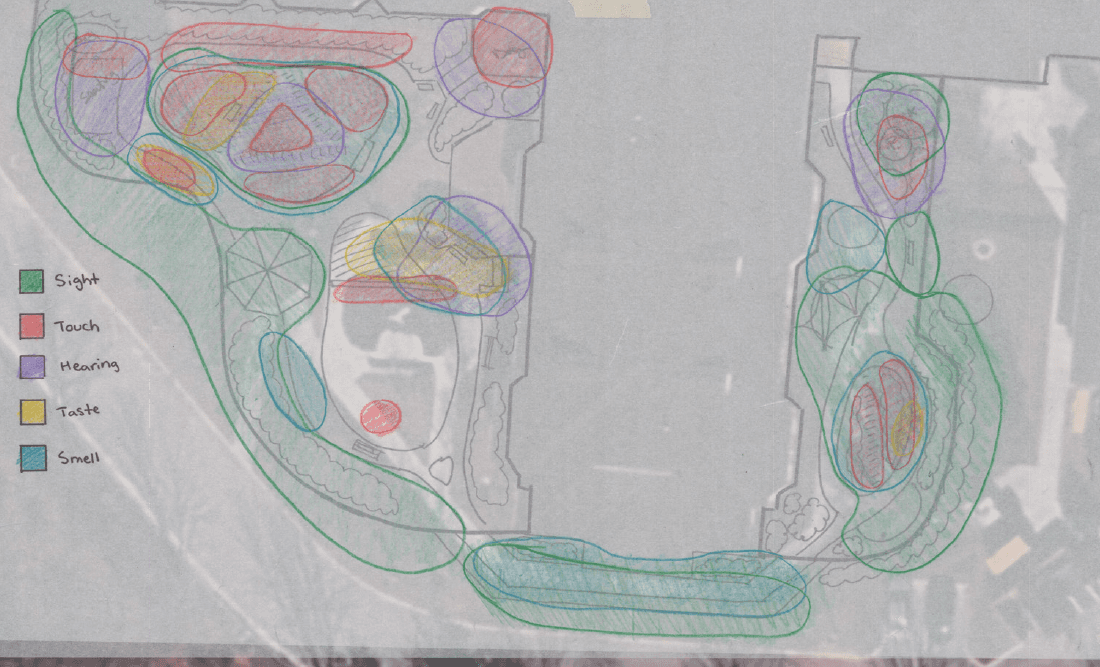
Senses Activated: Identifying the precise locations where biophilic responses, such as the scent of lavender or the sound of water, actively reduce stress and agitation.
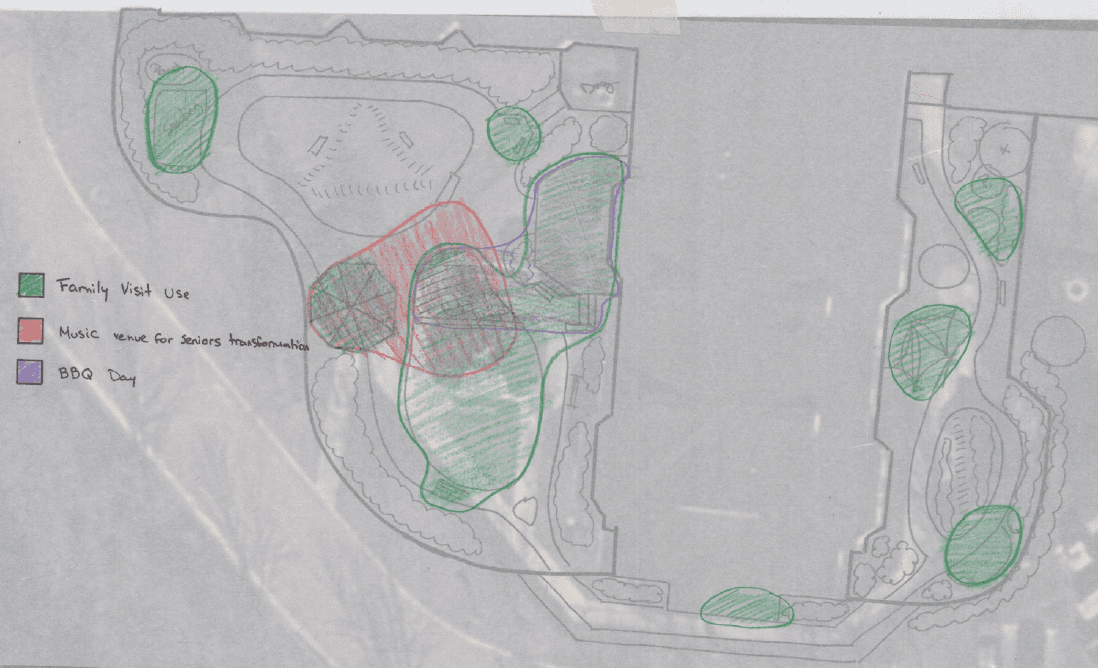
Event Usage: Visualizing the invisible social networks and cultural activities, like family visits or “Sunday BBQ," that the design is built to support.
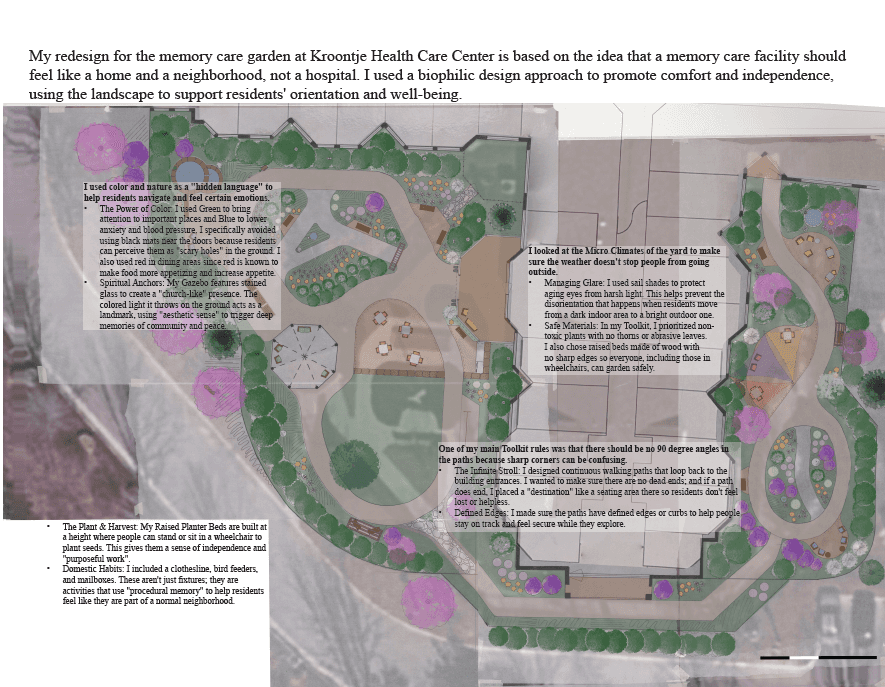
My redesign for the memory care garden at Kroontje Health Care Center is based on the idea that a memory care facility should feel like a home and a neighborhood, not a hospital. I used a biophilic design approach to promote comfort and independence, using the landscape to support residents' orientation and well-being.